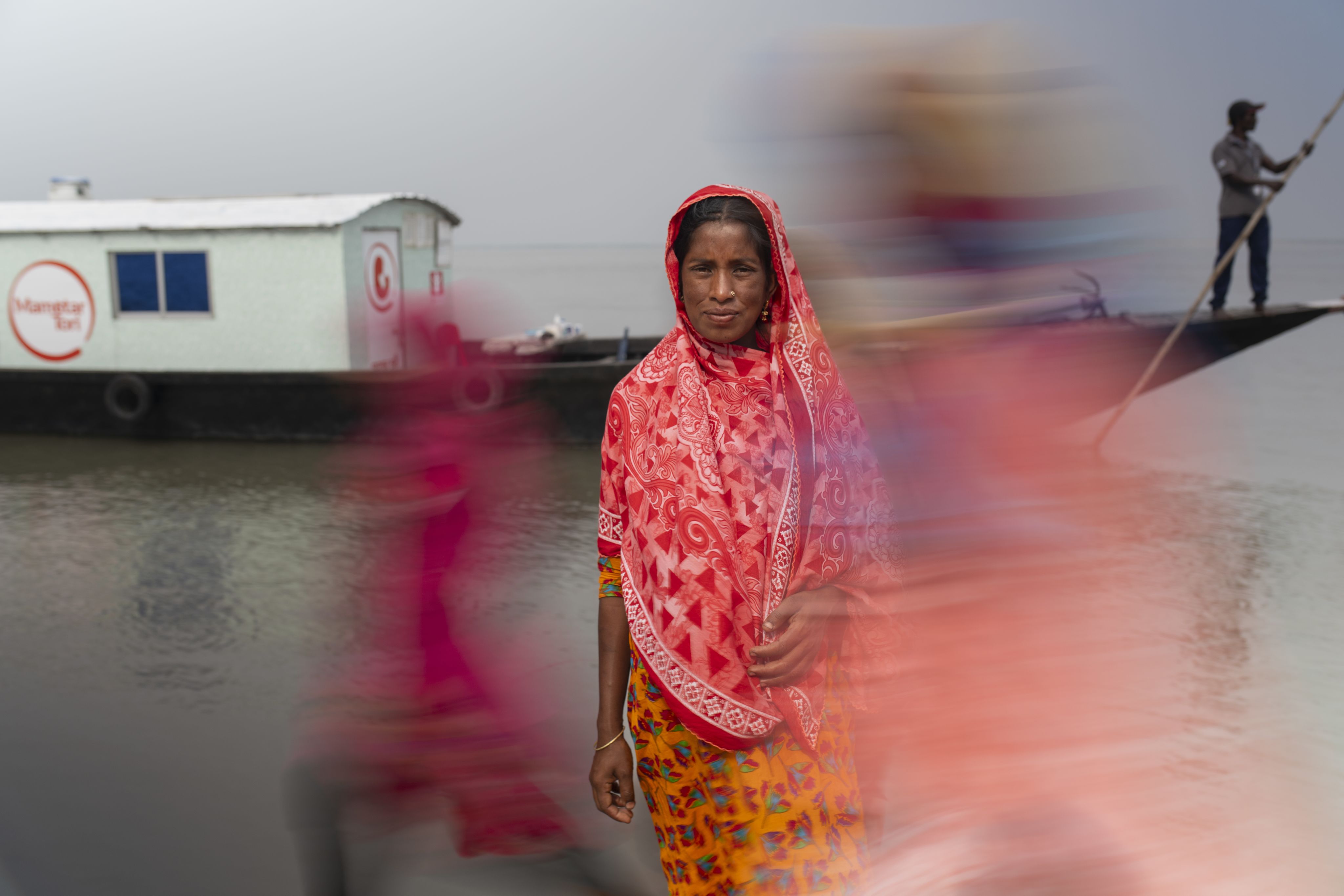5
innovative ways we’re keeping mothers and
babies healthy.
5
innovative ways we’re keeping mothers and babies healthy.

The day of birth is the most dangerous in a child's and the mother’s life.
Around half of newborn deaths and the majority of maternal deaths happen in this period.

2.4
MILLION NEWBORN BABIES DIE PER YEAR
Globally, there are an estimated 2.4 million newborn deaths per year and another 2 million are stillborn, with 40% of stillbirths occurring during labour.
6,000
NEWBORN BABIES DIE PER DAY
Every day, 6,000 newborn babies die – mostly from preventable causes like infection, premature birth, and complications during labour.
36
EVERY 36 SECONDS, A BABY DIES
Every year, 900,000 babies die during labour. That’s one baby every 36 seconds.
2
EVERY 2 MINUTES, A WOMAN DIES
Every two minutes, a woman dies from complications during pregnancy or childbirth.
The risk is highest in places of poverty and crisis. A child born in sub-Saharan Africa is 18 times more likely to die before the age of five than one born in Australia or New Zealand.
But with skilled midwives, medicine, clean water and safe places to give birth, mothers and babies can survive. Countries like Bangladesh, Kenya and Rwanda have made huge progress in newborn and maternal health over the last few decades, significantly reducing preventable deaths. We know there are solutions that have been proven to work.
That’s why Save the Children is delivering urgent care to mothers and babies around the world.
Scroll to read 5 innovative ways we are keeping mothers and babies healthy.
Bangladesh’s Boat of Affection.

Known as ‘Mamotar Tori, which translates as ‘the Boat of Affection’ in Bangla, our maternity boat travels to pregnant women in water-surrounded communities in Bangladesh who are unable to travel. Save the Children works alongside local partner SKS Foundation to bring midwives and medical supplies to remote villages by boat and aims to improve the access and the quality of maternal and newborn health, reducing the number of preventable deaths and increasing access to family planning.
Nargis’ story.
Save the Children midwife Nargis meets nine-month old Irfan*, who was delivered with the help of the Mamota Project, in Gaibandha.
I educate them about the risks of home-delivery… During the hospital delivery, we'll be there to see what is wrong and take the necessary steps needed to be done and save your life."
Nargis, a midwife at a satellite clinic run by Save the Children's Mamota project, checks a mother and her baby in Gaibandha, Bangladesh. Photo: Fatima Tuj Johora / Save the Children.
Nargis, a midwife at a satellite clinic run by Save the Children's Mamota project, checks a mother and her baby in Gaibandha, Bangladesh. Photo: Fatima Tuj Johora / Save the Children.
Her words are striking a chord with the villagers. More women are feeling confident to go to the health centre to deliver their baby, with support from a trained midwife like Nargis.
There are many challenges for women living in this area, Nargis explains:
This area is susceptible to natural disasters, with a cycle of droughts, floods, strong winds, and heavy rainfall. Additionally, there are issues with the roads, making transportation particularly challenging.”
The Boat of Affection provides a solution to ensure access to medical care, even in the most challenging circumstances.
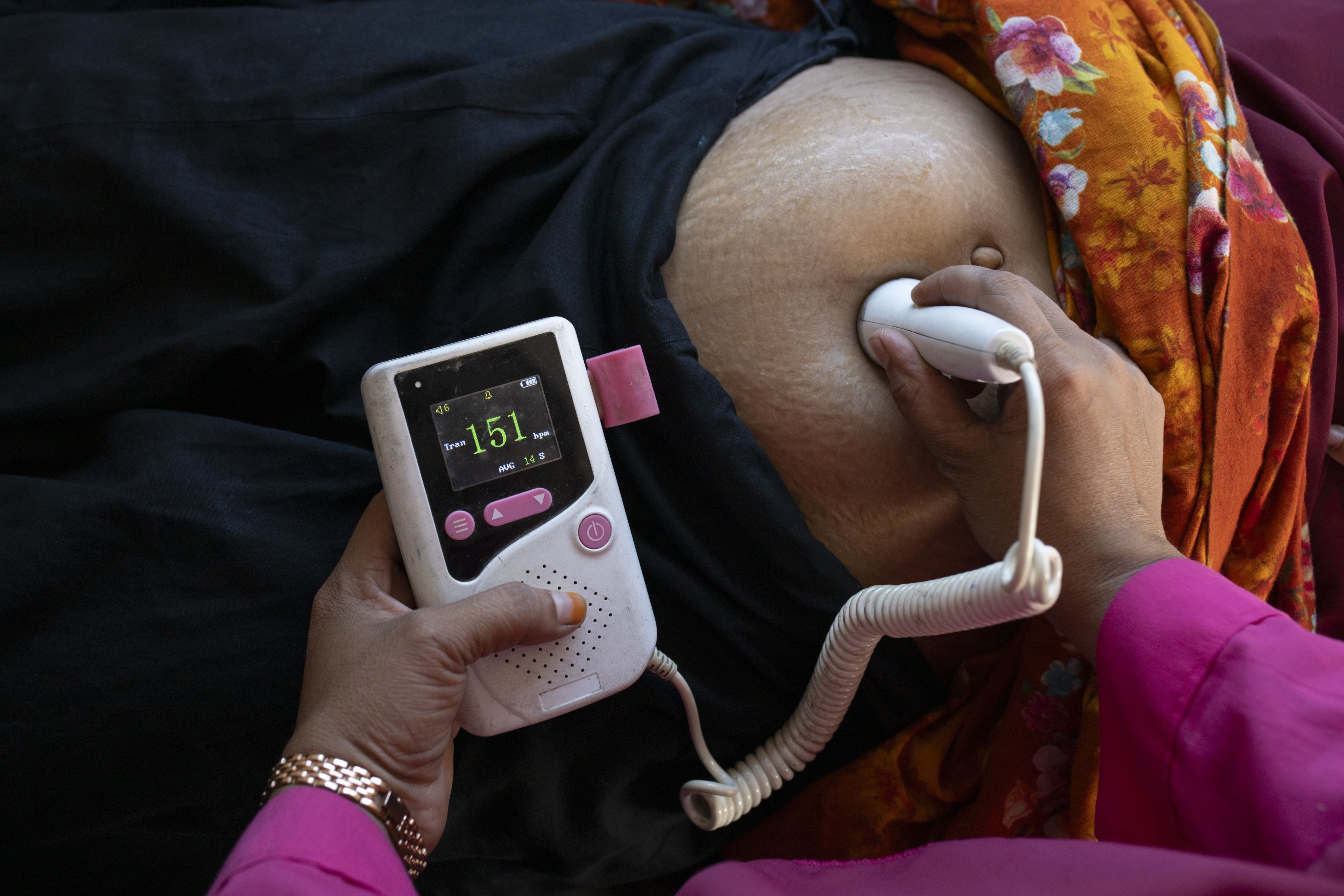
5-months pregnant Tisha* attends a check-up with Nargis, a midwife at a satellite clinic run by Save the Children's Mamota project to support Char communities in Gaibandha, Bangladesh. Photo: Fatima Tuj Johora / Save the Children.
5-months pregnant Tisha* attends a check-up with Nargis, a midwife at a satellite clinic run by Save the Children's Mamota project to support Char communities in Gaibandha, Bangladesh. Photo: Fatima Tuj Johora / Save the Children.
Sometimes we can't help a pregnant lady deliver and we have to refer her to a higher facility. But, since we have the Mamotar Tori, we are better off."
The Boat of Affection has become a lifeline for pregnant women during floods and emergencies, offering them a route to higher ground where they can receive specialist care.
Nargis strives for all women to have access to care:
I believe it's essential to have midwives in every district, especially in remote areas."
Rwanda’s drones that cover miles in minutes.

In Rwanda, Save the Children is working with drone company Zipline and the Ministry of Health to deliver medicine and blood directly to a health centre at Mahama refugee camp, the biggest refugee camp in Rwanda.
Prior to the health centre at the refugee camp, mothers experiencing complications in birth had to be driven to a town about 35 kms (24 miles) away along extremely bumpy, dirt roads, with the journey taking about 2 hours. Many women would arrive at the hospital in advanced stages of labour or have given birth during the journey, putting their own and their baby’s life at risk.
A drone packed with medical supplies and blood takes off at Zipline in Kayonza, Rwanda.
Now, Save the Children provides caesarean sections and blood transfusions on site at the Mahama Refugee Camp health centre and drone delivery of essential medicine and blood provides a rapid route to reach the health centre. This has been a game-changer for babies' and mothers’ lives and well-being, reducing infant and mother mortality as well as post-partum complications.
Lab technician Xavier collects the Zipline drone delivery at a medical facility run by Save the Children in Mahama Refugee Camp, Rwanda.
Lab technician Xavier collects the Zipline drone delivery at a medical facility run by Save the Children in Mahama Refugee Camp, Rwanda.
Each drone – or zip – can carry up to 1.6kg of medical supplies. That’s 3 x 500ml blood bags. The average time from order received to launch is 5 minutes.
They are fully autonomous electric delivery drones that travel through the air at up to 70mph. In an emergency, this means essential medicine or blood can be with those who need it within half an hour of ordering it.
Lab technician Xavier unboxes the Zipline delivery, inspects and registers the blood packages before refrigerating them.
Lab technician Xavier unboxes the Zipline delivery, inspects and registers the blood packages before refrigerating them.
Since Zipline started operating in Rwanda, the number of maternal deaths due to postpartum haemorrhage has halved, and the number of blood products wasted has been reduced by two-thirds.
Lab technician Xavier unboxes the Zipline delivery, inspects and registers the blood packages before refrigerating them.
Lab technician Xavier unboxes the Zipline delivery, inspects and registers the blood packages before refrigerating them.
Delivering life amid conflict in Gaza.

Save the Children’s Emergency Health Unit delivers lifesaving care in disasters. In Gaza, we established a maternity unit where women could access essential reproductive, newborn, and paediatric care.
Tima* (26) holds her one-day-old baby Lana* at Save the Children's maternity unit in Gaza.
My pregnancy was difficult, as I had back pain because we have to do everything on the ground – cooking, washing, sleeping. It was tough being pregnant during the war."
Tima’s* story.
Tima found out she was pregnant in July 2023. She was excited to be having her second child. She decorated a room in their home in preparation. She thought about how she would spoil her new baby with the best food and nice clothes.
Then, in October 2023, the war in Gaza started, and it changed everything. Tima and her family were displaced multiple times as violence spread across the Gaza Strip.
Tima shared how tough it was to be pregnant during the war.
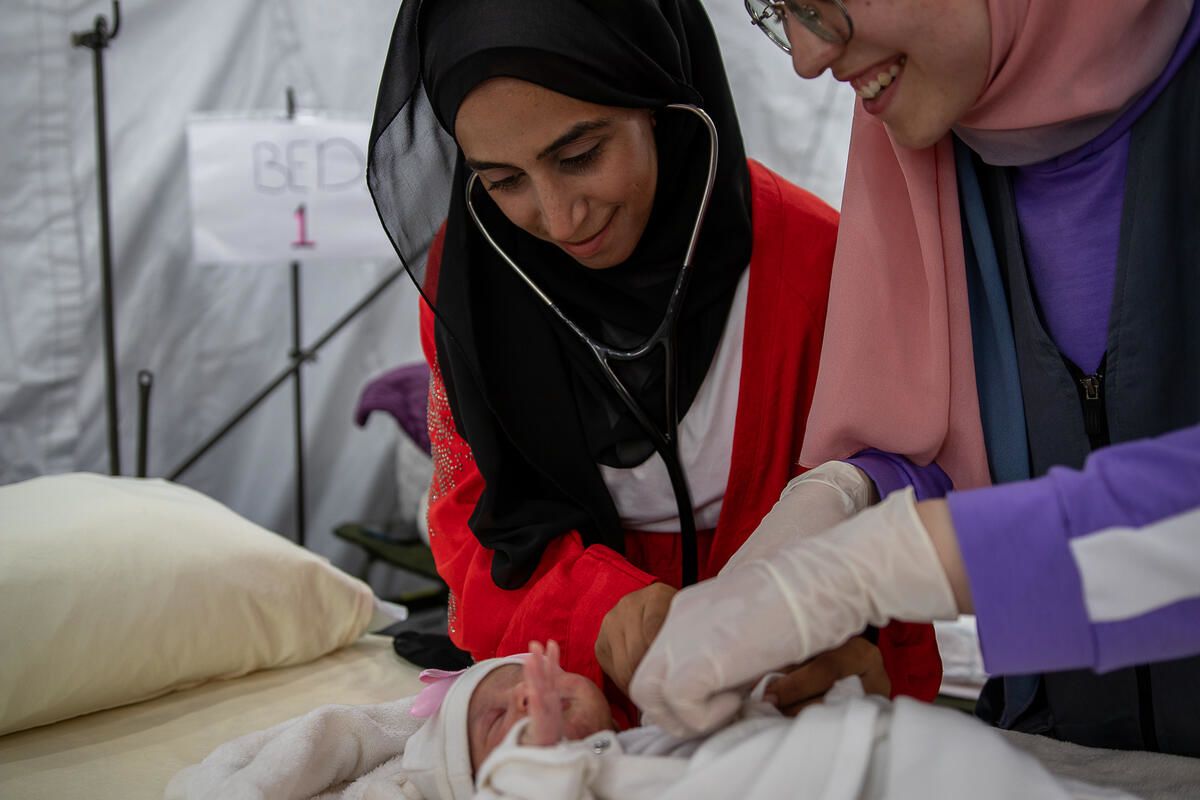
Save the Children midwife Deda* (24) with new mother Tima* (26) and baby Lana* (1 day). Photo: Sacha Myers / Save the Children.
Save the Children midwife Deda* (24) with new mother Tima* (26) and baby Lana* (1 day). Photo: Sacha Myers / Save the Children.
She was also worried about where she would give birth safely. She was worried about whether she would be safe in a healthcare facility, given the continuous attacks.
Tima visited the hospital where Save the Children provides life-saving services for children and their families for her prenatal check-up. She liked the facility and asked if she could give birth when she was due. Then, on 26 April 2024, Baby Lana* arrived safely. Baby Lana was the first of many babies to be born at Save the Children’s maternity unit in Gaza.
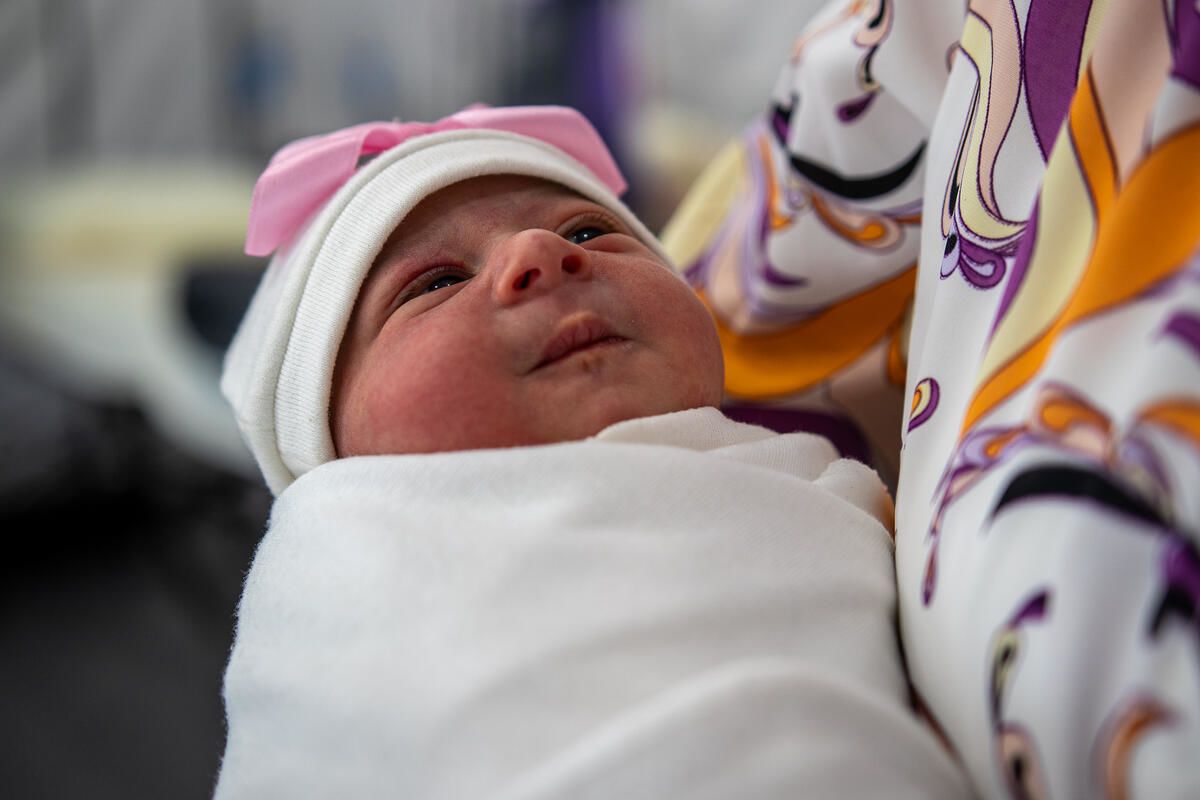
Tima* (26) holds her one-day-old baby Lana* at Save the Children's maternity unit in Gaza. Photo: Sacha Myers / Save the Children.
Tima* (26) holds her one-day-old baby Lana* at Save the Children's maternity unit in Gaza. Photo: Sacha Myers / Save the Children.
I was happy and grateful to find a place here (at the maternity to give birth). I had been here (the hospital) before and I liked it, so I asked to come here [for the birth].”
Although baby Lana was healthy when she left the hospital, after three days she developed a fever, refused to breastfeed and had blood coming from her umbilical cord. Tima was quick to bring her daughter back to the hospital, where the Emergency Health Unit treated her for sepsis. If left untreated, sepsis can easily kill a baby. The infection was due to the tough living conditions in the displacement camp where her family lives. Here, they have very limited access to clean water and washing facilities. However, with Tima’s quick action, a course of antibiotics and some close monitoring, baby Lana made a full recovery.
We used to have a whole room prepared for the baby with a bassinet and everything. Now, I’m worried about the insects and snakes in the tents and it not being safe for the baby. We wake a lot at night because we can’t secure the tent, and we sleep on the floor. I’ll protect her as much I can, as we protect ourselves. We hope it will be OK."
Eileen* (49) holds her one-day-old granddaughter Lana* at a Save the Children maternity unit, Gaza.
Eileen* (49) holds her one-day-old granddaughter Lana* at a Save the Children maternity unit, Gaza.
My message to other mothers (around the world) is for them to be grateful for what they have because here we have nothing. People overseas think we’re not clean or uneducated but it’s not like that. We never used to be like this."
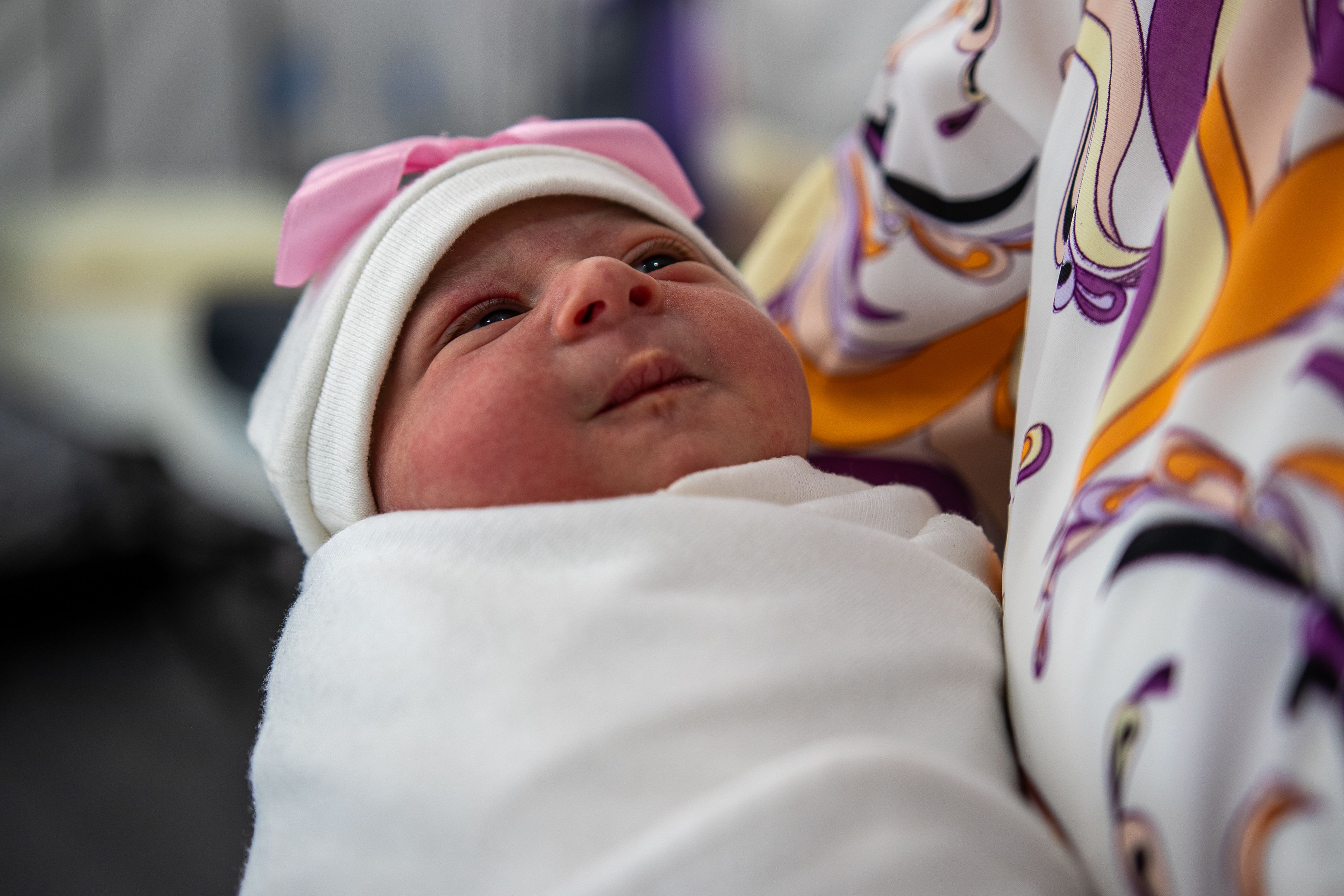
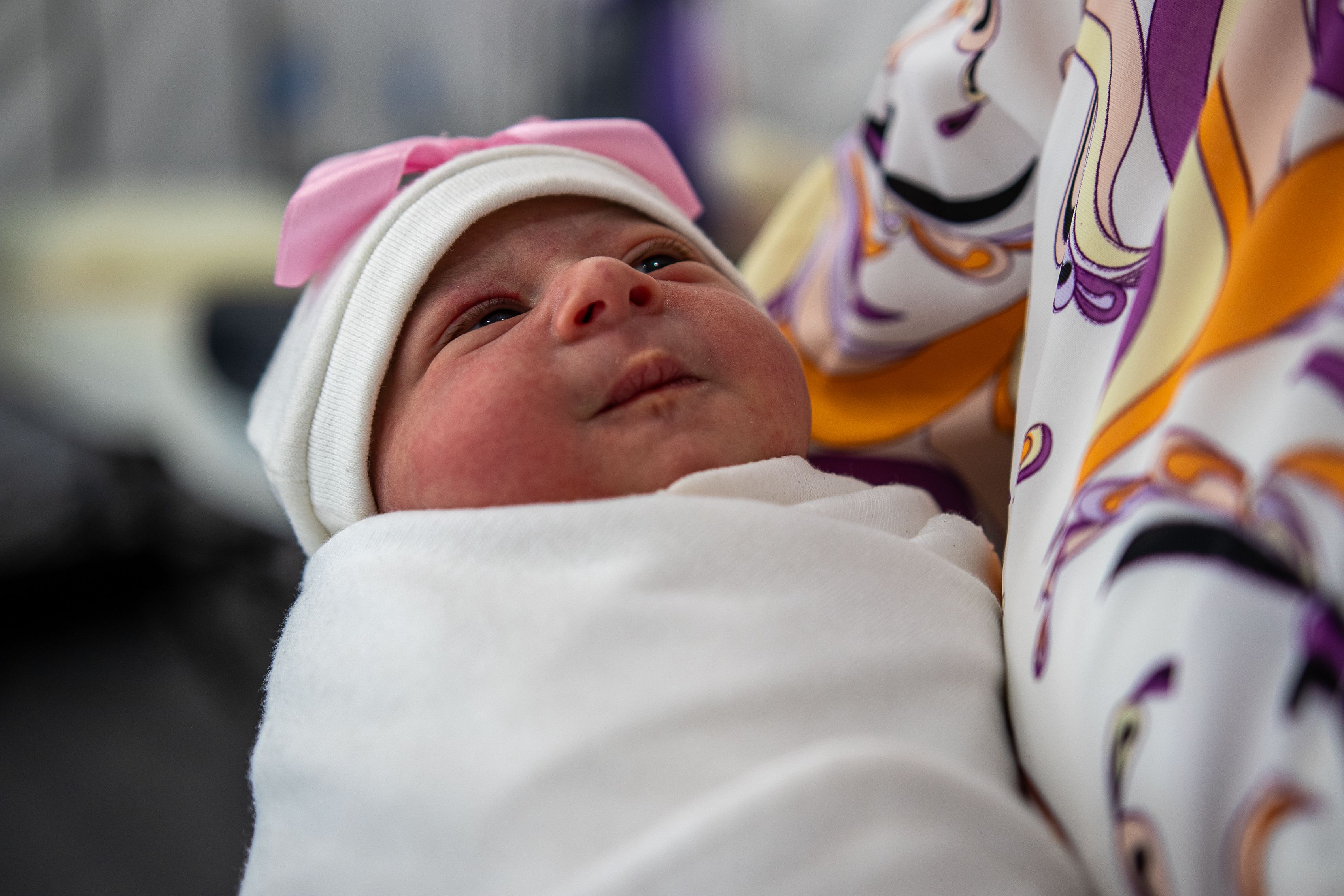
Donate now to our Children’s Emergency Fund, and you’ll help us reach mothers and newborns with lifesaving support in the most dangerous places to be born.
Together, we can help mothers and babies in the world’s toughest places.
Kangaroo mother care in Kenya.
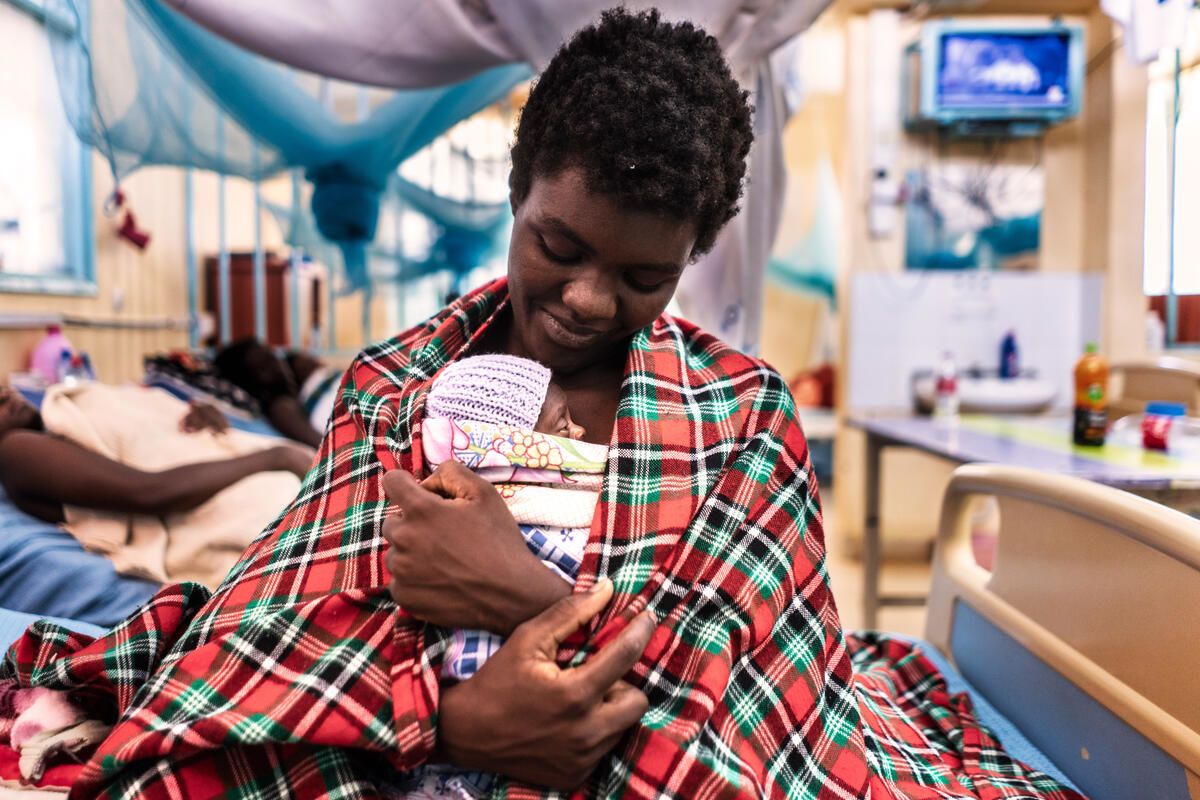
In Kenya, we worked closely with the Ministry of Health to establish Kangaroo Mother Care which involves skin-to-skin contact between the mother and baby, as a standard practice in the care of preterm and low birthweight babies.
Diana, 21, holding the hand of her newborn baby, Blessings, in the Kangaroo Mother Care ward at a hospital in Bungoma, Kenya.
Anytime a baby is in the Kangaroo Mother Care position there's that feeling of love, and they just feel stress-free."
Diana’s story.
Diana was told when she went into early labour that the chances of survival were low. She said:
I had no more hope."
Diana was transferred from her local health centre in Bungoma, Kenya, to a hospital with a specialist ward for premature births. When Diana’s baby, Blessings, was born, she weighed just 1kg.
The pair stayed in the Save the Children and the GSK-supported hospital for five weeks. During this time, Diana practised Kangaroo Mother Care with baby Blessings. Kangaroo Mother Care is a skin-to-skin connection between mother and baby, where the baby is held to the mother's chest using a sling for many hours.
Lilian, 32, holding her newborn baby in the Kangaroo Mothercare ward at a hospital in Bungoma, Kenya. Photo: Fredrik Lerneryd / Save the Children.
Lilian, 32, holding her newborn baby in the Kangaroo Mothercare ward at a hospital in Bungoma, Kenya. Photo: Fredrik Lerneryd / Save the Children.
Rosemary, an experienced midwife at the hospital, has been trained to support mothers with Kangaroo Mother Care. Rosemary explains:
A baby who is under incubator care, power can go off and this baby will become hypothermic. But a baby who is on their mother's chest, there is constant warmth. There is also bonding – a mother learns early enough to bond with the child."
Diana is determined to encourage other mothers in a similar position to her:
They need to have courage, they need to accept the situation and have hope."
Lilian, 32, holding her newborn baby in the Kangaroo Mother Care ward at a hospital in Bungoma, Kenya. Photo: Fredrik Lerneryd / Save the Children.
Lilian, 32, holding her newborn baby in the Kangaroo Mother Care ward at a hospital in Bungoma, Kenya. Photo: Fredrik Lerneryd / Save the Children.
Rosemary sometimes calls the practice Kangaroo Family Care and encourages any caregiver or family member to use it. She says:
Anytime a baby is in the Kangaroo Mother Care position there's that feeling of love, and they just feel stress-free."
From measurement to survival in Ethiopia.

We are trialling a new, community-based tool to help families and healthcare workers identify low-birthweight and premature babies by using simple body measurements, such as measuring newborn foot length.
Dr. Fitsum Belay monitors a newborn baby who is in the neonatal intensive care unit. Dr. Fitsum Belay is a Neonatologist and part of the newborn foot length research team.
If this tool was scaled up, it could help millions of babies to receive the care they need to survive and to be healthy."
In Ethiopia, 50% of newborns are born at home. Often, preterm and low birth weight babies who are born at home don't get the specialised care that they require for survival, leaving them at a higher risk of death.
Save the Children has partnered with Hawassa University College of Medicine and Health Sciences in Ethiopia to develop a simple community-based tool that uses a newborn's foot length to test as a reliable indicator for low birth weight.
The tool has been developed through rigorous research and using a Human-Centred Design approach. By simply measuring their newborn foot length, it enables mothers to identify whether their baby is at risk quickly, encouraging them to seek life-saving care within the first 24 hours of life.
A health worker measuring newborn foot length. Photo: Seifu Assegid/Save the Children.
A health worker measuring newborn foot length. Photo: Seifu Assegid/Save the Children.
Sarah Williams, senior maternal and newborn health advisor at Save the Children, explains the power of such a small and simple tool. She tells us:
There's a strong evidence base about the relationship between a baby's foot length, arm circumference and their weight at birth. This means that even when scales are not available to weigh a baby, it's possible to identify babies who are more likely to be low birth weight, simply by measuring their foot length or mid-upper arm circumference."
Mother Haymanot* gives feedback on a prototype tool for measuring newborn foot length. Photo: Hiwot Mekonnen/Save the Children.
Mother Haymanot* gives feedback on a prototype tool for measuring newborn foot length. Photo: Hiwot Mekonnen/Save the Children.
Based on this research and the lessons from previous teams that have worked in this field, we've been developing simple, affordable and scalable ways that can help mothers, their families and community health workers to recognise these low birth weight and preterm babies that are either born at home or in health facilities that are poorly equipped."
Father Addisu*, 25, tests one of the foot measuring tools on a doll provided by Save the Children. Photo: Hiwot Mekonnen/Save the Children.
Father Addisu*, 25, tests one of the foot measuring tools on a doll provided by Save the Children. Photo: Hiwot Mekonnen/Save the Children.
If this tool was scaled up, it could help millions of babies to receive the care they need to survive and to be healthy. We need this tool in Ethiopia. So does the rest of the world.”
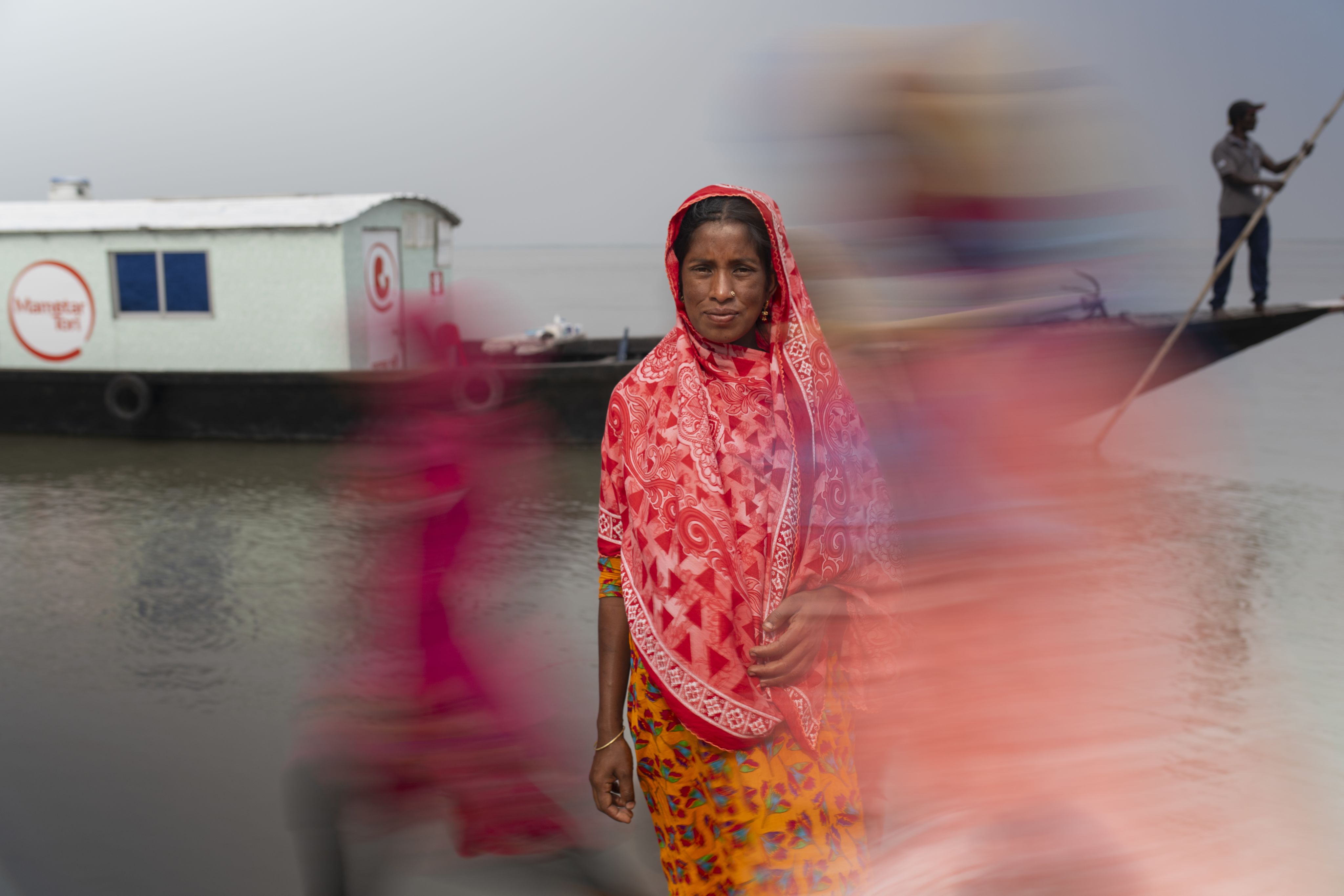
Can you imagine a child being born without safety, medicine or care?
For millions of babies born in conflict zones, refugee camps, or disaster-hit communities, there is no guarantee of survival. Every year, 900,000 babies die during labour. That’s one baby every 36 seconds.
The majority of newborn and maternal deaths are preventable. But unless we can reach more mothers with lifesaving care, countless babies will not survive their first days of life.
Donate now to our Children’s Emergency Fund, and you’ll help us reach mothers and newborns with lifesaving support in the most dangerous places to be born.
Together, we can help mothers and babies in the world’s toughest places.
Every baby deserves a safe start in life.